You might wonder if your insurance would pay for treatment if you have varicose veins. In this article, you will discover a few varicose vein-related conditions that most insurance plans may cover.
What does "medical necessity" mean, and why does it matter?
Health insurance companies frequently use the term "medical necessity" to assess if the patient's coverage covers a specific test or treatment. Nevertheless, what does the phrase "medical necessity" really signify? To put it briefly, the word "medical necessity" refers to the need for a specific course of therapy.
Several variables determine the necessity of a treatment from a medical standpoint.
- First things first: There must be proof that the treatment is successful, i.e., that it can improve the patient's medical condition.
- Second, the treatment course must suit the patient's condition and be customized to meet their needs.
- Third: The course of therapy must be clinically acceptable, meaning that it must be proven safe and effective while having advantages that outweigh the risks.
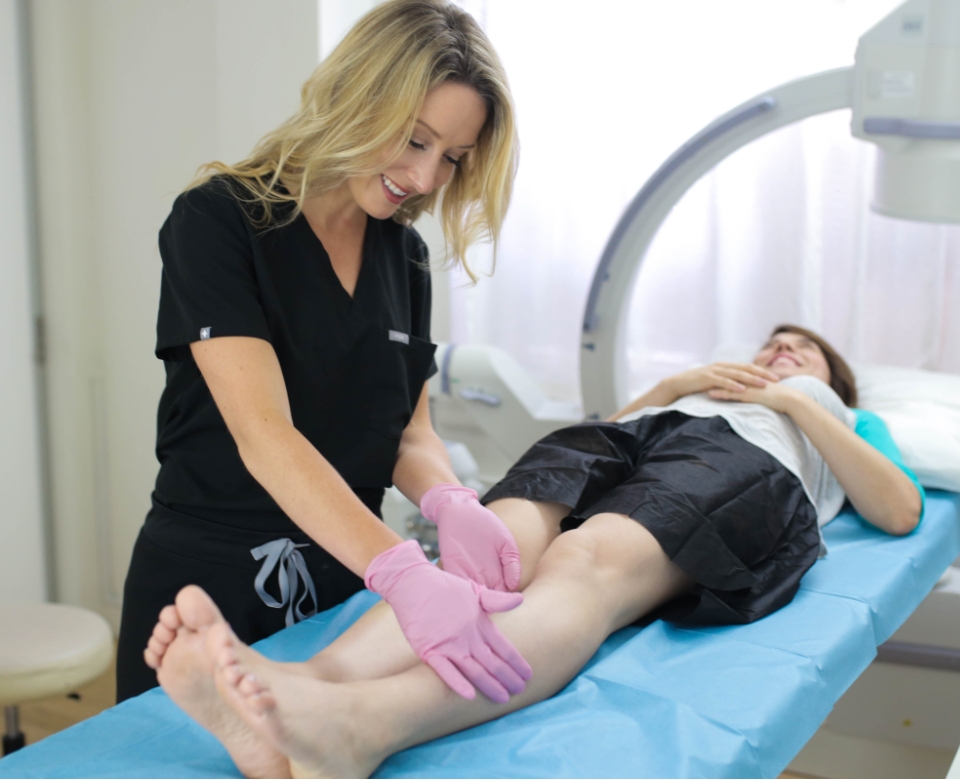
Does insurance cover the treatment of varicose veins?
Varicose veins are a cosmetic problem for a lot of people. However, for some people, they may cause pain and even worsen existing health issues. Are Varicose Vein Treatments Covered by Insurance? The severity of your ailment and your particular insurance plan are two variables that determine the answer to this query.
Most insurance companies view varicose vein treatments as cosmetic or elective. Therefore, it's unlikely that your expenses will be reimbursed. Let's say, however, that you are dealing with continuous swelling, soreness, discomfort, or discolouration of the skin. If so, your physician might be able to identify a condition known as "chronic venous insufficiency," which is covered as a medical necessity.
Now that you know this, you may wonder what doctor treats varicose veins. The issue can be treated with a vascular surgeon or phlebologist specializing in treating veins and blood vessels.
Prior Consent and Monetary Obligation
Patients could still have to go through a prior authorization process even if insurance coverage for varicose vein therapy is authorized.
The insurance company controls every step of this procedure, and we assist patients in navigating it. The easier this process is, the more actively the patient represents himself to their insurance company.
How to Determine Your Eligibility
Initially, you can check to see if treatments for varicose veins are covered by reading your insurance policy. As long as you match the other requirements, most of the time, there is no reason why they shouldn't be covered unless they are expressly prohibited.
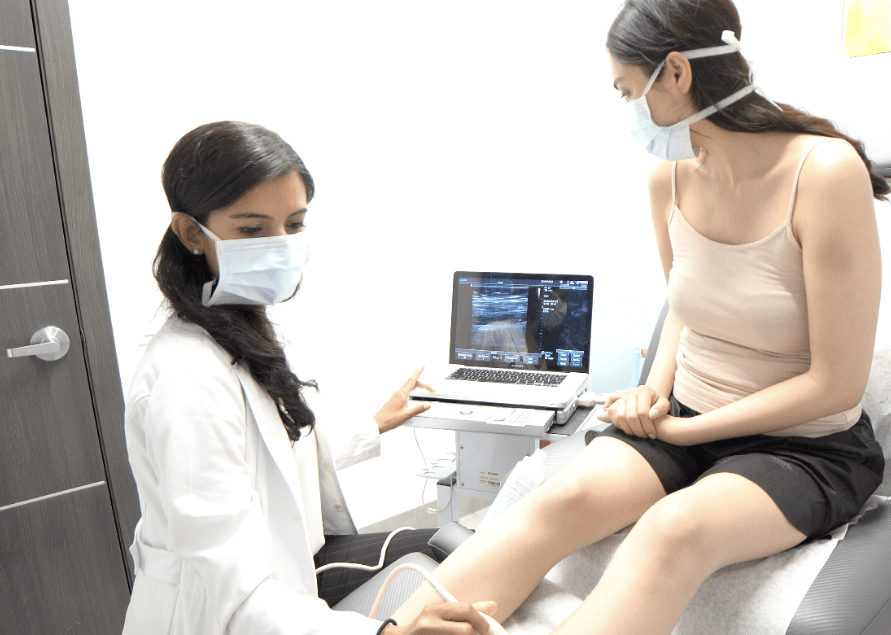
Usually, you need to go for a medical consultation. Your insurance will determine your eligibility for funding depending on the results. You typically need a letter of reference from your general practitioner to attend this consultation.
It's also doubtful that your private insurer will approve a consultation and treatment on the same day, which is a crucial consideration.
Many will want to examine the scan findings before obtaining treatment authorization.
In a nutshell
Our specialists are pleased to discuss the best course of action and check if your insurance covers varicose vein treatment if you're dealing with any of the diseases mentioned above.
Treating varicose veins is a speciality of our board-certified vein experts. They can help you create a personalized therapy plan that will enable you to regain your sense of self.